updated June 26, 2025, previously titled
How smoking and sun affect skin’s look and feel
Skin health and beauty- big business
Browse social media or news sites online and you notice skin health and appearance is a priority for most people. Sales for skin care and appearance products and services is a multi-billion dollar industry. If you’re on social media, you’ve probably seen posts from friends who are involved in direct selling companies for skin care, maybe you are also.
As a family physician, I treated skin problems frequently. Some of these are primary skin problems, but some are the result of lifestyle habits, other medical conditions, and even medical treatments. While some of these may be unavoidable, others are preventable.
This post will look at two avoidable risks to skin health and appearance-smoking and ultraviolet light.
Skin Deep- cells and layers
First let’s take a deeper look at our skin, it’s more complex than you may realize. It has two layers-
the top layer, the epidermis
the lower layer, the dermis
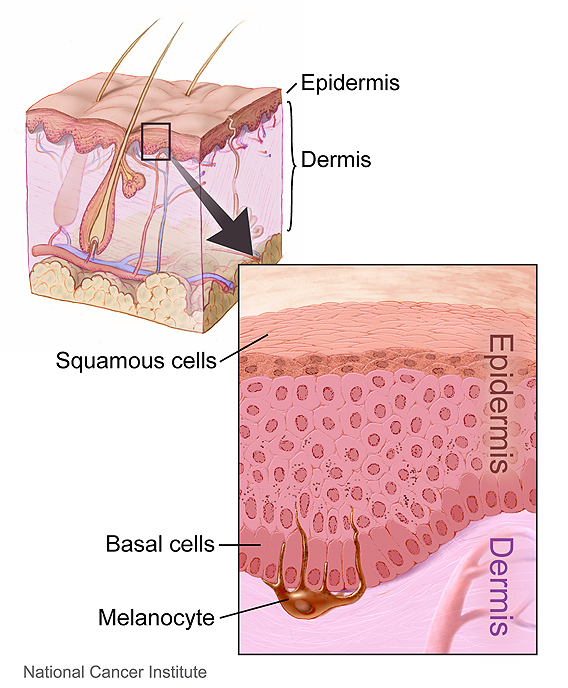
- The layers of the skin (epidermis and dermis), as well as an inset with a close-up view of the types of cells in the skin (squamous cells, basal cells, and melanocytes). Source: National Cancer Institute Creator: Don Bliss (Illustrator) This image is in the public domain and can be freely reused. Please credit the source and, where possible, the creator listed above.
Skin disease and trauma involve damage to one or both layers of the skin- the dermis or epidermis, or to the individual cells- squamous cells, basal cells, or the melanocytes-the cells with pigment that give our skin color.
Cancers can develop in any cell of the skin. Melanoma is cancer of the melanocytes.
(This photo is for illustration only and should not be used to diagnose a skin lesion. See a physician if you have a skin lesion that concerns you. )

- a melanoma skin lesion-Source: National Cancer Institute Creator: Unknown Photographer- This image is in the public domain and can be freely reused. Please credit the source
Smoking and Your Skin
I’ve previously discussed 7 reasons to be smoke free. One of those is skin health.
By decreasing circulation, smoking robs skin of nourishment and oxygen; this weakens skin , making it susceptible to infection, cancer, and aging.
Skin experts wrote in the Journal of Dermatological Science
“Smoking is associated with many dermatological (skin) conditions, including
- poor wound healing,
- premature skin aging,
- squamous cell carcinoma and melanoma,(cancers)
- acne,
- psoriasis, and
- hair loss

Tobacco’s Effect on Skin
- Facial wrinkles and furrows (eg, crows’ feet at corners of the eyes, smoker’s lines around lips)
- Baggy eyelids and slack jawline
- Uneven skin coloring: grayish, yellow with prominent blood vessels (telangiectasia)
- Dry, coarse skin.
Long term, the skin of a 40-year-old heavy smoker will resemble that of non-smoking 70-year-old. !
Other potential hazards from tobacco use include
- increased risk for bacterial, yeast, and viral skin infections
- impaired circulation increasing the risk of frostbite, Raynaud’s syndrome, and blood clots (thrombosis)
- thrush and gingivitis
DermNet NZ offers this gallery of photos illustrating these ways tobacco use can damage our skin. ALERT: These photos are graphic.
Tips to Become Smoke Free
- Know what triggers you to smoke. Do you smoke after a meal, while driving, or when you’re stressed? Make a plan to handle each trigger.
- Consider getting support from 1–800–QUIT–NOW or smokefree.gov
- You can buy nicotine gum, patches, and lozenges from a drug store.
- Remove cigarettes, ashtrays, and lighters from your home, office, and car.
- Remind yourself of the benefits of quitting.
- Even if you start smoking regularly again, don’t give up. Most people who smoke need a few tries to quit before finally being successful.
- Talk to your healthcare provider about other resources to help you quit.
Ultraviolet Light Effects on Skin
Basking in sunlight may enhance our mood, but too much can damage our skin.
The signs of photo-aging are obvious to physicians-
- yellowing or sallowing of the skin complexion
- dry and rough texture with wrinkling,
- unevenly pigmented skin tone with dilated blood vessels.
- stretched out
- easy bruising
Visit this link from the Canadian Dermatology Association to see what photoaged skin looks like
Photoaging
Photoaging is premature aging of the skin caused by repeated exposure to ultraviolet radiation (UV), primarily from the sun but also from artificial UV sources, such as tanning beds. Besides aging, excess sun exposure can cause
- Burns
- Rash due to increased sun sensitivity when taking certain medications
- Cancers- skin cancers are the most common type of cancer.
How to Limit UV Light Exposure
- Use a broad spectrum sunscreen, SPF 15 or higher
- Wear hats, sunglasses, sun protective clothing
- Avoid sun exposure, especially from 10 am to 4 pm
- No tanning bed use.
When selecting a sunscreen, make sure the label says:
- Broad spectrum: The words “broad spectrum” means that the sunscreen can protect your skin from both types of harmful UV rays — the UVA rays and the UVB rays.
- SPF 30 or higher: The American Academy of Dermatology recommends that you select a sunscreen with an SPF rating of 30 or higher.
- Water resistant: Dermatologists also recommend that you look for the words “water resistant.” This tells you that the sunscreen will stay on wet or sweaty skin for a while before you need to reapply. Water resistance lasts either 40 or 80 minutes. Not all sunscreens offer water resistance.
Exploring the HEART of Health
I’d love for you to follow this blog and follow me on social media.
I share information and inspiration to help you transform challenges into opportunities for learning and growth.
Add your name to the subscribe box to be notified of new posts by email. Click the link to read the post and browse other content. It’s that simple. No spam.
I enjoy seeing who is new to Watercress Words. When you subscribe, I will visit your blog or website. Thanks and see you next time.
Dr. Aletha
- About Dr. Aletha
- How to Use this Site
- Make Your Life Easier
- Search by Category
- Share the HEART of health
- my Reader Rewards Club
- RoboForm Password Manager
The cover image of this post was created by JetPackAI available with WordPress.

- We all care about our appearance, including this cute monkey. Photo by Andre Mouton on Pexels.com









