This information is current as of the date of original publication or update but may have changed by the time you read this. Do not use this information for diagnosis or treatment purposes. Before making health decisions, discuss with a qualified healthcare professional.
Imagine you consult a physician for a problem. The doctor asks you questions and examines you. Then you have blood tests, cultures, X-rays,a CT scan or MRI. You hope these tests show what is “wrong” so the doctor can treat you.
But what if all the tests are “normal”? Normal tests suggest that your symptoms may be due to a cause for which there is no biomarker.
A biomarker is a diagnostic test that indicates a specific disease or condition.
biomarker-A biological molecule found in blood, other body fluids, or tissues that is a sign of a normal or abnormal process, or of a condition or disease.
Both physicians and patients would like a biomarker for every disease. But many common conditions do not yet have a biomarker.
These include migraine, fibromyalgia, irritable bowel syndrome, Parkinson’s disease, many skin conditions, Alzheimer’s dementia, depression, and other psychiatric disorders.

For these disorders, physicians make a “clinical diagnosis”.
clinical diagnosis-The process of identifying a disease, condition, or injury based on the signs and symptoms a patient is having and the patient’s health history and physical exam
Much of medical research is devoted to finding biomarkers for these and other conditions. This article from KFF focuses on finding biomarkers for psychiatric disorders, especially depression. Such tests could be helpful not only for diagnosis but also for guiding therapy.
But there are potential downsides, like cost, insurance coverage, privacy, and potential discrimination, as explained in the article.
Psychiatrists’ Use of Biomarkers Could Open a New Window Into Mental Health Diagnoses
by Jamie Ducharme, March 17, 2026
Amanda Miller was 30 and pregnant with her second child in Hershey, Pennsylvania, when she developed depression. After she gave birth, her depression worsened. It was joined by a slew of unexplained health problems.
Miller, a neuroscientist, said she saw several psychiatrists and got prescriptions for drug after drug. Over two years, she tried four antidepressants and two antipsychotics. None of that helped — until her primary care doctor noticed high levels of an autoimmune marker in her blood.
A specialist then ran “every test in the book,” Miller said. Eventually, she was diagnosed with the autoimmune disease lupus and prescribed an inflammation-lowering steroid. Some of her symptoms let up within hours. Her depression subsided not long after.
“I was convinced it was a placebo effect,” Miller said, “but then it kept working.”
Had inflammation been contributing to her mental health problems all along? Miller thinks so, although she can’t know for sure. Her psychiatrists never raised that possibility, she said.
Laboratory vs Clinical Diagnosing
In most medical specialties, doctors can confirm whether to pursue a type of treatment through tests, such as blood work, imaging, and biopsies. Mental illnesses, however, have historically been diagnosed and treated based on outward symptoms. That could change.
The American Psychiatric Association in a January paper included ideas for how it might incorporate biomarkers — biological indicators of mental illness that could show up on diagnostic tests — into future versions of its Diagnostic and Statistical Manual of Mental Disorders.
The DSM, sometimes called “psychiatry’s bible” because of its influence in the field, provides criteria for diagnoses. It’s used by clinicians assessing patients and by insurance companies deciding whether to cover care.
‘Coordinated’ Research Needed
Psychiatric biomarkers are not ready for widespread use yet, the paper emphasized. Scientists have researched the topic for decades, with little to show for it.
More research is needed to prove these metrics are valid and reliable enough to be used in patient care, the APA’s paper said, and other researchers have raised questions about how their use could affect health care costs, insurance coverage, and patient privacy.
Adding biomarkers to the DSM would be “a very big deal,” said Jonathan Alpert, an author of the January paper and vice chair of the APA’s Future DSM Strategic Committee.
Access to test results, along with symptoms, could streamline insurance coverage decisions and help clinicians make faster and more accurate diagnoses and treatment recommendations, he said. If patients’ biology suggested they’d respond better to one treatment than another, their doctor could waste no time in starting there.
A Prescribing “Crapshoot”
Currently, prescribing psychiatric medications can be “a bit of a crapshoot,” with clinicians unable to predict whether they will work for a particular patient, said Matthew Eisenberg, director of the Center for Mental Health and Addiction Policy at the Johns Hopkins University Bloomberg School of Public Health.
In a seminal, early 2000s trial funded by the National Institute of Mental Health, about 30% of the study’s participants with depression saw symptoms disappear with their first antidepressant treatment. That study is still one of the most robust antidepressant trials conducted — although researchers have more recently argued that fewer people are cured by these medications than its results suggest.

Such a trial-and-error approach can lead to ineffective and unnecessary prescriptions, a topic of attack by proponents of the Make America Healthy Again movement, spearheaded by Health and Human Services Secretary Robert F. Kennedy Jr. Kennedy has been especially critical of antidepressants, having linked them to violence after a mass shooting without evidence and blaming doctors for overprescribing medications for children.
HHS is analyzing psychiatric diagnosis and prescription trends and evaluating alternative mental health treatment approaches, with a particular focus on children, spokesperson Emily Hilliard said in a statement. Hilliard did not respond to a question about Kennedy’s previous comments.
Biomarkers are already used to guide treatment in other medical disciplines, such as oncology. Arizona, Georgia, Kentucky, Texas, and more than a dozen other states require insurers to cover such testing. Blood and imaging tests are now used to help diagnose Alzheimer’s disease as well.
A Future for Psychiatric Biomarkers
The APA included in its article a variety of ways psychiatric biomarkers could be used in the future — such as testing for brain activity, genetic profiles, or immune markers associated with certain psychiatric conditions, including schizophrenia and substance use disorders.
In depression, for example, about a quarter of patients have elevated levels of an inflammatory protein, called C-reactive protein, that can be found through a blood test.
Research has shown that people with high levels of this protein seem to respond better when given drugs that alter dopamine levels in the brain, rather than using only selective serotonin reuptake inhibitors, or SSRIs, a common type of antidepressant.
C-reactive protein still needs to be “robustly validated” as a biomarker, but it’s among the most promising currently under investigation.
APA
A “coordinated, well-funded” research effort is needed to achieve such validation, the APA wrote — a tenuous prospect since the Trump administration slashed funding for research.
The National Institute of Mental Health alone had at least 128 grants, worth almost $173 million, canceled in 2025, according to a research letter in the journal JAMA. Though some grants have since been restored, researchers relying on federal money still fear their work is vulnerable to cuts.
“There’s a great need for continued, active funding of research related to mental health,” Alpert said, but scientists will have to grapple with “uncertainties of the funding landscape.”
Ripple Effects on Coverage, Costs
Health care costs tend to be higher among patients with poorly controlled mental illnesses, due to expenses like hospital visits, outpatient appointments, and prescriptions. Some research suggests biomarker testing could save money by landing on the right treatments faster and avoiding some of these costs.
One modeling study estimated that testing to look for genetic components that may influence a drug’s effectiveness could save the Canadian health system $956 million over 20 years if used among adults with major depression in British Columbia. Another study, by Spanish researchers, found that such testing reduced costs for most of the 188 participants with serious mental illness.
Whether the same would be true in the U.S. health care system is unknown. In the short term, Johns Hopkins’ Eisenberg said, an approach that uses biomarkers could raise health care spending due to the costs of testing.
Insurers may decline to cover pricey biomarker tests, It takes a while for new science to be proven safe and effective,
Matthew Eisenberg, Johns Hopkins
And once it is, insurance companies don’t cover it immediately.”
“The Beginning of a Revolution”
Some researchers have raised concerns that insurers or employers could discriminate against people whose biological profiles suggest they’re at risk of developing serious neuropsychiatric conditions.
It’s a “critical moment” to consider legislative approaches to protect patients and train clinicians about how to appropriately use these tools, said Gabriel Lázaro-Muñoz, a member of Harvard Medical School’s Center for Bioethics.
“I do not think that the field of psychiatry is currently ready to manage this,” he said.

The mental health system isn’t ready to “jump in with both feet,” said Andrew Miller, a professor of psychiatry and behavioral sciences at the Emory University School of Medicine, who studies inflammation-related depression. But the APA’s embrace of biomarkers signals “the beginning of a revolution,” he said.
“This is a recognition … that what we’ve done up to this point has not been good enough,” Miller said. “And we can do better.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
This article first appeared on KFF Health News and is republished here under a Creative Commons Attribution-NoDerivatives 4.0 International License.![]()
Depression
Depression is common among people who have a chronic disease such as cancer or diabetes. Fortunately, depression is treatable even if you have another medical illness or condition. Learn more about chronic disease and depression: Caring for your mental health #shareNIMH

Biomarkers in Cancer Care
Biomarker testing is a way to look for genes, proteins, and other substances (called biomarkers or tumor markers) that can provide information about cancer. Each person’s cancer has a unique pattern of biomarkers.
Some biomarkers affect how certain cancer treatments work. Biomarker testing may help you and your doctor choose a cancer treatment for you.
There are also other kinds of biomarkers that can help doctors diagnose and monitor cancer during and after treatment. To learn more, visit the Tumor Markers fact sheet.
Biomarker testing is for people who have cancer. People with solid tumors and people with blood cancer can get biomarker testing.
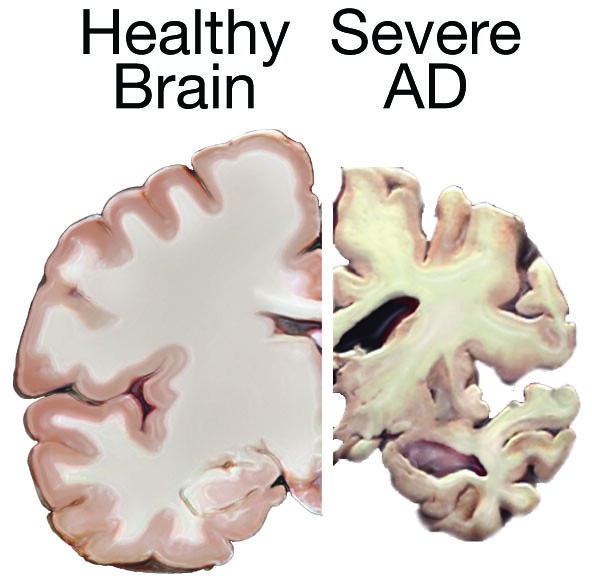
The FDA-approved blood tests for diagnosing Alzheimer’s disease
In May 2025, the U.S. Food and Drug Administration (FDA) approved the first blood test as a tool to help diagnose Alzheimer’s disease. The test is called Lumipulse.
The test measures certain proteins, including a specific form of the tau protein. This can indicate amyloid plaques in the brain, a protein that is considered the hallmark sign of Alzheimer’s disease.
This blood test, along with other diagnostic tools can help diagnose Alzheimer’s disease. While the blood test can detect changes even before memory problems begin, it is only recommended for use in people showing symptoms of Alzheimer’s disease.
The test is still being refined and can’t diagnose Alzheimer’s disease on its own.
What to Remember from this Post
I learned from the KFF article and the references, did you? What are your takeaways from what you read? Here are some to consider.
- Doctors use laboratory tests and imaging to supplement information gleaned from talking to and examining patients.
- Biomarkers for common conditions make diagnosis easier and more precise, and help guide therapy.
- Discovery of biomarkers for other serious conditions will help patients get earlier diagnosis and more effective treatment. More research is needed.
- New medical discoveries introduce trade-offs in cost, payment, benefit, and potential misuse.
How will you use what you’ve learned? How may you apply this information to a current or future health concern?
What more information do you need and where will you find it?

Exploring the HEART of Health
I’d love for you to follow this blog. I share information and inspiration to help you transform challenges into opportunities for learning and growth.
Add your name to the subscribe box to be notified of new posts by email. Click the link to read the post and browse other content. It’s that simple. No spam.
I enjoy seeing who is new to Watercress Words. When you subscribe, I will visit your blog or website. Thanks and see you next time.
Use this search box for related posts on this blog or other topics of interest to you.