updated January 27, 2026
This post was originally written and posted 2 years before we had even heard of SARS-CoV-2, aka COVID-19. Four years later, “flu” symptoms are just as likely to be due to COVID as influenza, maybe more so. Still, we need to be vigilant because neither has disappeared. This post focuses on influenza.
To many people “the flu” is any respiratory illness characterized by some combination of fever, cough, congestion, headache, fatigue, and body aches. That term has become so nonspecific even we doctors use it that way.
But, correctly, it refers to influenza, one of many viruses that cause illness. The illnesses caused by the other viruses are “colds”, upper respiratory infections, aka URIs, bronchitis, pharyngitis, sinusitis, and pneumonia.
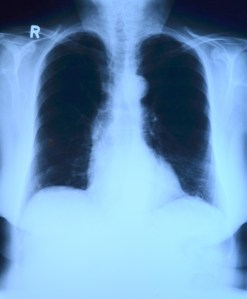
Before the rapid flu test, using a nasal swab, we doctors diagnosed influenza by the characteristic symptoms, confirmatory findings on exam, and knowing there was an outbreak in the community.
The test is not absolutely necessary but is helpful for confirmation in the event the illness doesn’t progress as expected or to differentiate it from other illnesses, especially COVID.
Vaccination-key to prevention
The World Health Organization (WHO), Centers for Disease Control and Prevention(CDC) , the National Foundation for Infectious Disease and every other reputable medical organization recommends vaccination against influenza.
My family and I always get vaccinations which have successfully protected us without side effects or adverse reactions. There are risks, as is the case for any medical procedure, or other things we do in life. In this case we have decided the benefit outweighs the risk.
Other tips to stay well and protect others
- Stay home if you are sick, and ask your family, co-workers and employees to do the same.
- If you absolutely must go out among other people, put an effective mask over your nose and mouth.
- Cover your nose and mouth when coughing or sneezing
- Wash your hands frequently.
- Clean frequently touched surfaces.

Antiviral (influenza) medications
Tamiflu
The antiviral drug Tamiflu, generic oseltamivir, will “shorten the duration and severity of symptoms” by 1-2 days, if started early (within 24-48 hours). There is some evidence that it will also lessen the risk of serious complications , especially in higher risk people (see below ).
I warn people that even with Tamiflu they will still feel miserable for a few days. But if it gets you back to school or work a day earlier, it may be worth the cost.
Oseltamivir can also be prescribed for prevention, if you know you have had close contact with someone with confirmed influenza, such as a household member. It’s only effective though for that episode, a 10 day course taken as soon as possible after exposure.
Xofluza
Xofluza, generic baloxavir, is for treatment of uncomplicated influenza for children and adults 12 years and older, who have been sick for no more than 48 hours. Patients take 2 tablets as a single dose. It can also be used post exposure .
Relenza
Relenza, generic zanamivir, is a dry powder that is inhaled twice daily for 5 days or daily for prevention
Peramivir
Peramivir (Rapivab): A single-dose intravenous (IV) injection for 6 months and older, typically only used for patients needing admission to a hospital .
Home care of influenza
- Rest; eat and drink as normally as possible; extra fluids if running a fever
- Non-prescription cough/congestion /pain/fever meds
Don’t confuse Tamiflu (generic oseltamivir) a prescription anti-viral drug with Theraflu, an over the counter drug that treats symptoms.Theraflu does not affect the course of the illness.
Here are more general guidelines on what to do if you get a respiratory illness from FamilyDoctor.org.
Flu complications
Influenza causes uncomfortable disabling symptoms but most people recover fairly quickly and fully. In some cases influenza can progress rapidly and overwhelm the respiratory and/or nervous systems, leading to death.
People also die from complications of influenza, and infants, young children and the elderly have greatest risk.The most common fatal complication is bacterial pneumonia, infection in the lung.
Influenza can also attack the nervous system causing brain inflammation (encephalitis and/or meningitis) and paralysis in the form of Guillain Barre syndrome .
High risk persons-take influenza seriously
Persons with chronic illnesses like diabetes, lung disorders, chronic liver or kidney disease, depressed immune systems and cancer , as well as infants and persons of advanced age are at greater risk of complications and should always consult a physician if feeling ill. If you are not sure if you fall into that category, ask your doctor.
Exploring the HEART of Health
I’d love for you to follow this blog. I share information and inspiration to help you transform challenges into opportunities for learning and growth.
Add your name to the subscribe box to be notified of new posts by email. Click the link to read the post and browse other content. It’s that simple. No spam.
I enjoy seeing who is new to Watercress Words. When you subscribe, I will visit your blog or website. Thanks and see you next time.