updated August 1, 2025
August is a strange month. It’s the only month without a major holiday in the United States. Although the temperatures still feel hot and muggy, by the end of the month, students and teachers are back in school and college for the “fall” semester. (Of course, if you are south of the equator, your experience may look quite different.)

Back to school, back to books
The main goal of school is education and reading is vital; books are the basic building blocks. That’s why Dolly Parton gives books away- read why here.
Inspiring Dreams: Dolly Parton’s Imagination Library
Inspired by a childhood story and personal struggles, Dolly Parton established the Imagination Library, providing free books to children. Her own experience led to the song “Coat of Many Colors,” conveying the value of love over material possessions. Through this initiative, she aims to nurture children’s dreams through the joy of reading.
Keep readingHow much do you know about medicine?
Speaking of school, there are always tests. Here’s one for you. Find out how much you know about medicine by taking this quiz that I wrote especially for blog readers.
Can medical knowledge make you a better patient? Take this quiz.
The purpose of board certification is to make sure you, the patient, are getting the best care possible from a physician.
Keep readingFriday Night Lights
Along with school comes sports. Although some go on year-round, many are tied to the school year, and football starts first in most places.
Even folks who don’t have a tie to a particular school adopt their local school’s team and follow faithfully. Fifty-plus years after my first football game as a college freshman, I still follow my team, the University of Oklahoma Sooners.
“Play like a champion today”
The OU Sooners football program has won 7 national championships and 7 players have received Heisman trophies. More importantly, the team never fails to show their fans exciting, hard-fought games. Even when they lose, they do so with plays that keep us guessing what’s going to happen next and wondering how such talented athletes can end up with the losing…
Keep readingSore Throats and Sneezing
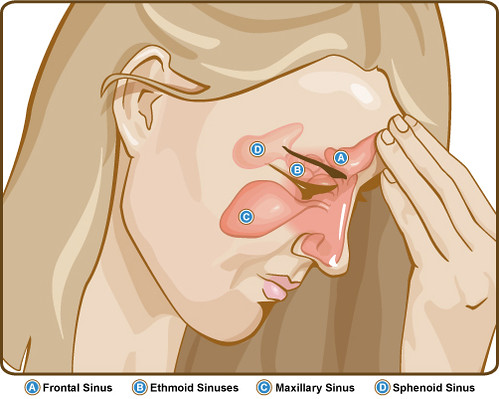
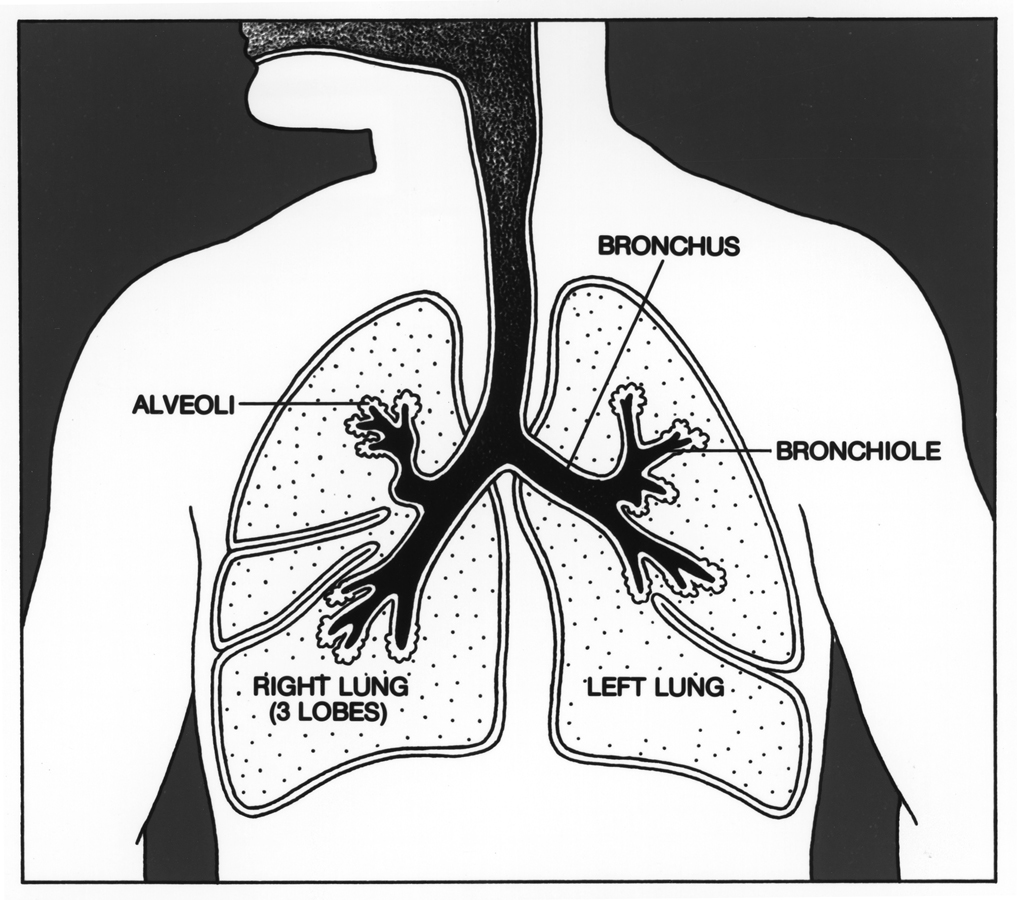
Although we think of colds and flu as winter illnesses, doctors start seeing patients with respiratory symptoms soon after school starts.
Places where people spend time together, like classrooms and dormitories, are prime places for people to share the viruses and bacteria that cause strep throat, colds, influenza, and COVID-19.
But there are steps we can take to lower the risk of exposure and illness. Check out the info in this post.
Head into the flu season with these 6 tips
We should all take influenza and COVID-19 seriously; consider my suggestions, talk to your personal doctor, keep up with recommendations from your local public health professionals, and do your part to keep your family and community well.
Keep readingExploring the HEART of health
As the season changes, ask yourself these questions about changes you might want or need to make in your life.
- What one activity can I start or improve to nurture my wellbeing?
- How is social media helping or hindering my growth as a person?
- What new or improved skill will make my life easier or more productive?
I’d love for you to follow this blog and follow me on social media.
I share information and inspiration to help you transform challenges into opportunities for learning and growth.
Add your name to the subscribe box to be notified of new posts by email. Click the link to read the post and browse other content. It’s that simple. No spam.
I enjoy seeing who is new to Watercress Words. When you subscribe, I will visit your blog or website. Thanks and see you next time.
Dr. Aletha
- About Dr. Aletha
- How to Use this Site
- Make Your Life Easier
- Search by Category
- Share the HEART of health
- my Reader Rewards Club
- RoboForm Password Manager
Help Watercress Words share the HEART of health

My Reader Rewards Club is a great way to earn free books and Bibles for yourself, friends, and family! Your journey to earning free faith-based products starts HERE.
(When you sign up through these links, I can earn free books too.)
As a member, you’ll have access to inspiring literature, Bibles, special promotional offers, and much more. Earning points is easy—you’ll receive 25 points just for signing up!
Watercress Words Bookstore
Bookshop.org is an online bookstore that financially supports local, independent bookstores.
We believe bookstores are essential to a healthy culture and they are dedicated to the common good.
Bookshop.org donates a portion of every sale to independent bookstores.