Call me weird, but I enjoy reading obituaries because I enjoy learning about people. Some obits revel in listing the person’s achievements-education degrees, military service medals, business positions, public and volunteer service recognition;descriptions of exotic travel, unique hobbies, special interests, creative pursuits and talents.
One of my favorite obits was different; simple, yet revealing a wealth of information about a man known simply as Jim (edited slightly for privacy)
“Jim, who died at 90 years old, was born on Valentine’s Day. He grew up on a farm, joined the Army, and went to a state teacher’s college on the GI Bill.
There he met his wife, and they had 2 children and 5 grandchildren. He earned a master’s degree and spent his professional life as a teacher of math, science, and social studies to elementary students. After retirement, he continued working as a tutor.
Jim enjoyed backyard gardening, walking to the library, math problems, weather reports and local high school sports. Jim always put the needs of others before himself.
In lieu of flowers please plant a flower, a tree, or even a vegetable garden. Jim would really like that.”
Despite his obituary’s simplicity, I feel like I knew Jim, he was someone I would have liked, even having as a neighbor. Obits don’t have to be complicated and fancy, and neither does life, if Jim is any proof.
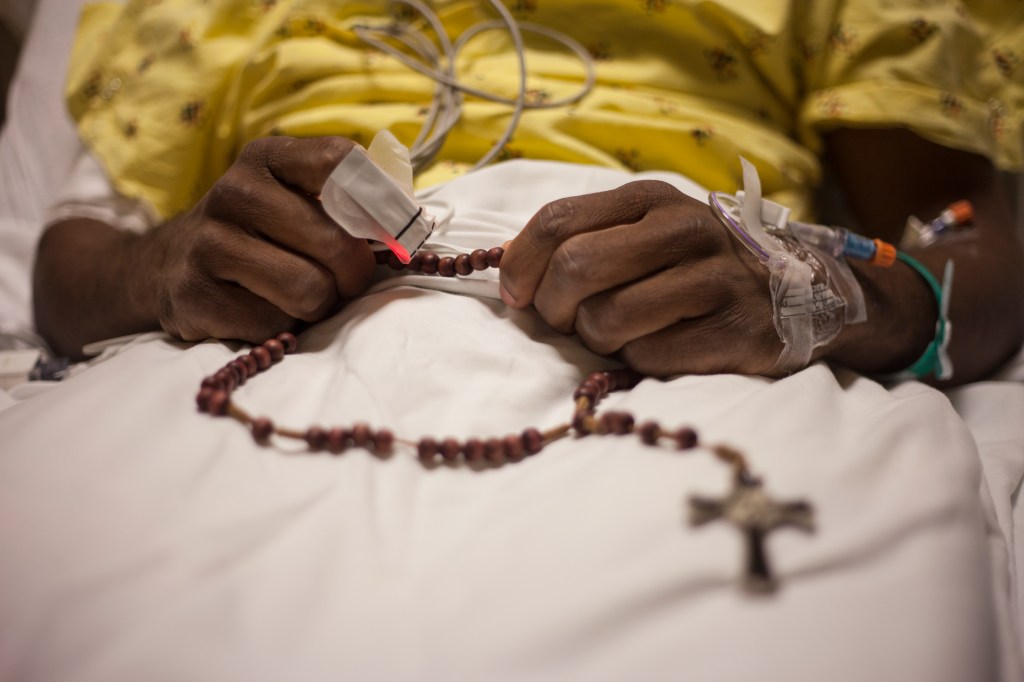
Unfortunately, death can be complicated. For some of us, a life-threatening or terminal health situation forces us to face death and if we’re wise, to prepare ourselves and our family . In other cases, unprepared families are left to deal with it while also grieving.
I have reviewed these two books that help us and our families make dying and death less arduous than it inevitably is. They cover the practical, financial, and social aspects of dying, as well as the medical, emotional, and spiritual aspects. Read them before you need them-because we all need them eventually.
Living life, facing death-a review of A Beginner’s Guide to the End
Even as a physician, I was surprised at the claim that only 10% to 20% of us will die without warning. The rest of us will know we have something that will likely take our life. And even if we don’t, we all know we will die eventually, although we tend to think and act…
Keep readingDying with Ease- a book review
Dr. Spiess doesn’t suggest that confronted with terminal illness we refuse treatment and give up. He advocates thinking about and planning for the dying process long before we develop an illness that might be fatal.
Keep readingexploring the HEART of health
I’d love for you to follow this blog and follow me on social media.
I share information and inspiration to help you transform challenges into opportunities for learning and growth.
Add your name to the subscribe box to be notified of new posts by email. Click the link to read the post and browse other content. It’s that simple. No spam.
I enjoy seeing who is new to Watercress Words. When you subscribe, I will visit your blog or website. Thanks and see you next time.
(This and other posts on this blog contain affiliate links that may pay a small commission to this blog if you make a purchase. )

Thanks,
Dr. Aletha