One of my all time most viewed posts is a story about my friend Pam and her weight loss journey using the Weight Watchers program. After successfully reaching and maintaining her weight goal, she started coaching others who have been equally successful. Recently, she was honored for 5 years as a coach.

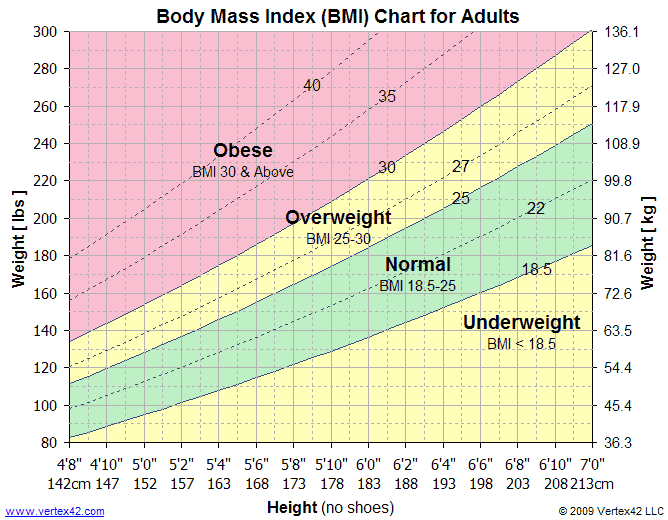
Many of us would like to weight less than we do, but some people struggle with severe excess weight that threatens their health and keeps them from enjoying life as they would like. These are usually people whose BMI, body mass index, is 30 or more. For people with diabetes, heart disease, liver disease, and osteoarthritis, even lower BMI can put them at excess disease risk.
The United States Preventive Services Task Force, USPSTF, recently reviewed weight loss methods and made a recommendation to physicians about how to help patients with weight.
The Task force encourages doctors to refer patients for “intensive, multicomponent behavioral interventions” to successfully lose weight.
What exactly does “intensive, multicomponent” mean?
A Patient Page in JAMA explains it this way- Interventions that are
- done in a group or individual setting, provided in person or virtually, and use print or online materials
- occurs over 1 to 2 years and with 1 to 4 sessions per month
- includes counseling about nutrition and exercise as well as education about how to self-monitor both of these components.
- includes help to identify barriers to weight loss, and help with problem solving related to challenges
- support from other people who are also working on weight loss
- education focused not only on weight loss but also on weight maintenance after interventions are completed.
Here is a link to the page-
Behavioral Interventions for Weight Loss


I haven’t used Weight Watchers but from what I understand about it, this is the type of program they offer. I’m not necessarily promoting WW, as they are called now, but if you want to lose weight I suggest looking for a program that includes these features. It certainly has worked for Pam and those she coaches.
“If we want to be people’s partners in what healthy means to the, it has to be about more than just weight. It has to be a total approach to how they can live their healthiest, best lives.”
Mindy Grossman, CEO of WW, quote taken from TIME magazine, October 15, 2018
And here is my story about Pam and her break-up with junk food.
How I “broke up” with junk food
and fell in love with healthy eating.
Meet my friend Pam. My husband and I met Pam and her husband in a ballroom dance class. I was immediately captivated by her radiant smile and Southern charm. Since then I have learned more about her and watched an amazing transformation in her life.

Pam graduated summa cum laude with a Bachelor of Arts from Mississippi State University in 1980. With a major in Communications, she started her career as a writer and Account Executive for advertising and public relations agencies in Mississippi and in Oklahoma where she moved after marrying. She was the Marketing Director for a large medical clinic for several years. Since 1995, she has enjoyed being a stay-at-home mom with involvement in PTA, church and community. In 2012, she was named Volunteer of the Year by her community public school system.
But despite such a charmed life, there was a struggle, one that Pam shares with many people. In this blog I have discussed the physical and emotional consequences of excess weight; you will be encouraged by Pam’s success story which she so generously shares with me and you.
“Breaking up is hard to do. ” By Pam Whitson
“I was happily married to the love of my life and should have been having the time of my life. Sadly, my self-confidence and my happiness had been stolen, and I was the thief.
For over two decades, I robbed myself of peak energy, vitality, health and beauty by totally disregarding my intake of food. Oh, don’t get me wrong, I thought about what I should do. I spent money on self-help tapes, gym memberships and weight loss programs from the practical to the extreme. I whined and wished about it constantly. And it didn’t help knowing that I was not alone; almost half of adults are overweight or obese.
And I had occasional moments of success. Like the time I was within four pounds of leaving the “obese” category. (Obese is a BMI, body mass index, of 30 or higher) After months of hard work, I ran to Glamour Shots for the mid-1990s version of a sequin and big hair make-over. On the way home from my triumphant photo session, I stopped by my favorite barbecue place and started eating my way right back to where I was before. I gained all the weight I had lost back and more.
I joked my way through feelings of depression, because I had an unhealthy relationship with food. I thought about it way too much. I ran to it for instant gratification. I was too in love with the tastes, the textures, the sheer delight of food. Even now, I love to grocery shop. One of my favorite places on the planet is the cereal aisle of the grocery store.

Finally, at age 53, after twenty years of carrying way too much weight for my 5’7 ½” (1.7 meters) (yes, the half inch counts!) frame, I was ready for a change. Really ready. Change isn’t easy. Change hurts. I walked into Weight Watchers and pretended it was my first time ever. I read everything. I listened and participated. I went to every meeting. I hung around afterwards and pestered my leader for every little nugget of information I could cling to.

I rejoined Weight Watchers in July, 2012, with 20 pounds (9 kg) still off from a previous Weight Watcher effort. I lost 40 pounds (18 kg) in 4 1/2 months to be at goal before Thanksgiving! I learned to maintain this loss during the required six week maintenance period with Weight Watchers and became an official Lifetime Member before the year’s end of 2012. This meant a lot to me because my birthday is New Year’s Day. How wonderful to start the year at a healthy weight!
At Weight Watchers I learned I could change. I could change what I put in my grocery basket. I could change what I ordered in restaurants. I could change how much I moved.
I could change my relationship with food for good.
I still enjoy food. Very much. Maybe even more than before because now I appreciate my food as fuel to live a healthy and active and even beautiful (in the eyes of the beholder) life! I still enjoy the tastes, even more so because I choose only the best. My plate is colorful with roasted veggies and fresh fruits and salad greens. I enjoy grilled lean chicken, steak and seafood. My carbs are high fiber, full of flavor and texture. I no longer long for the processed foods full of white flour, sugar and fat.
By pairing healthy eating with increased physical activity, I changed my weight dropped from 226 lbs (102 kg) to 150 lbs (68 kg). Now 70 pounds (31 kg) lighter and at a healthy BMI of 23, I feel so much happier and healthier.
But once I started eating better, even before I was near my goal weight, my self-esteem and confidence were instantly restored. Just knowing that I had a plan gave me optimism and excitement. I’ve been at goal for almost three years and I wouldn’t trade it for the world (or even a crisp cookie). And I now stay about 10 pounds (4.5 kg) below goal as a safety net.

In addition to my daily walks, I enjoy ballroom dancing, Jazzercise, swimming and an occasional bike ride. I wear a Fitbit and accomplish 15,000 steps a day.
I’ve been a Weight Watcher leader for two and a half years and just LOVE it! I never imagined I would do this; you might as well as told me I would become an astronaut. While helping me stay at a healthy weight, I enjoy the privilege of making new friends and helping other people be their most confident and healthy selves.
Just for fun, I’ve started a Park Walking group that explores different parks in our city every two weeks. We took a summer break (Oklahoma gets real hot in the summer) but will be back on the trails in September. Along with my awesome Weight Watcher members, I’m enjoying a new healthy relationship with food for good. ”

Weight Watchers may not be the answer for everyone, but Pam’s idea of changing our relationship with food should be a part of any weight management plan. Our eating habits affect our health in other ways, so even if you are not overweight, using food appropriately is important.
Physical activity has health benefits beyond weight loss. I joined Pam’s walking group and find it a fun way to exercise and make new friends. (My favorite walking shoe is Go Walk by Skechers.) In addition to social dancing with our husbands, Pam and I were in a ladies dance team. We performed a Western theme dance routine to the song “These Boots are Made for Walking” . That’s so appropriate for someone who walked her way from a BMI of 35 down to 25. If she can do it, so can you.
( This post contains affiliate product links; purchase through these links pays a commission to this blog; thank you)
Our son introduced my husband and I to Hello Fresh delivery meal kits and we’ve enjoyed the convenience, taste, variety, and quality. The meals feature lots of fresh vegetables with vegan and “fit” choices. We think we are eating healthier and ever with less work. Here is a link through which you can get $40 off your first order.
Thanks for letting me introduce you to my friend Pam. We would love to hear your weight management stories. Please share in the comments or send me a message if you want it kept anonymous. Remember, support from others is an important step toward success.
Dr. Aletha





