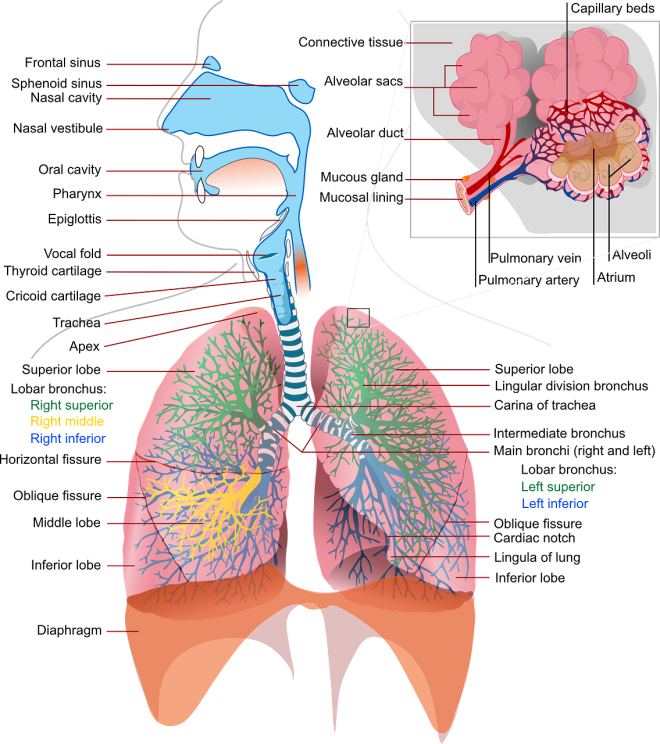
Even though IBS, irritable bowel syndrome, is a common gastrointestinal disorder, medical science still cannot fully explain its origin or understand the best way to treat it. But physicians can do much more to help patients with this condition than previously thought.
This information is current as of the date of original publication or update but may have changed by the time you read this. Do not use this information for diagnosis or treatment purposes. Before making health decisions, discuss with a qualified healthcare professional.
This article has been updated March 13, 2021.
What is IBS?
Recurrent abdominal pain or discomfort averaging 1 day per week for 3 months associated with
- altered bowel movements
- change in frequency of stool
- change in form or appearance of stool
- not explained by other conditions that are known to cause similar symptoms
IBS patients may have any combination of pain, diarrhea, and constipation, which can alternate or go in remission at times. Other common symptoms include
- passage of mucus
- increased gas
- bloating and/or fullness
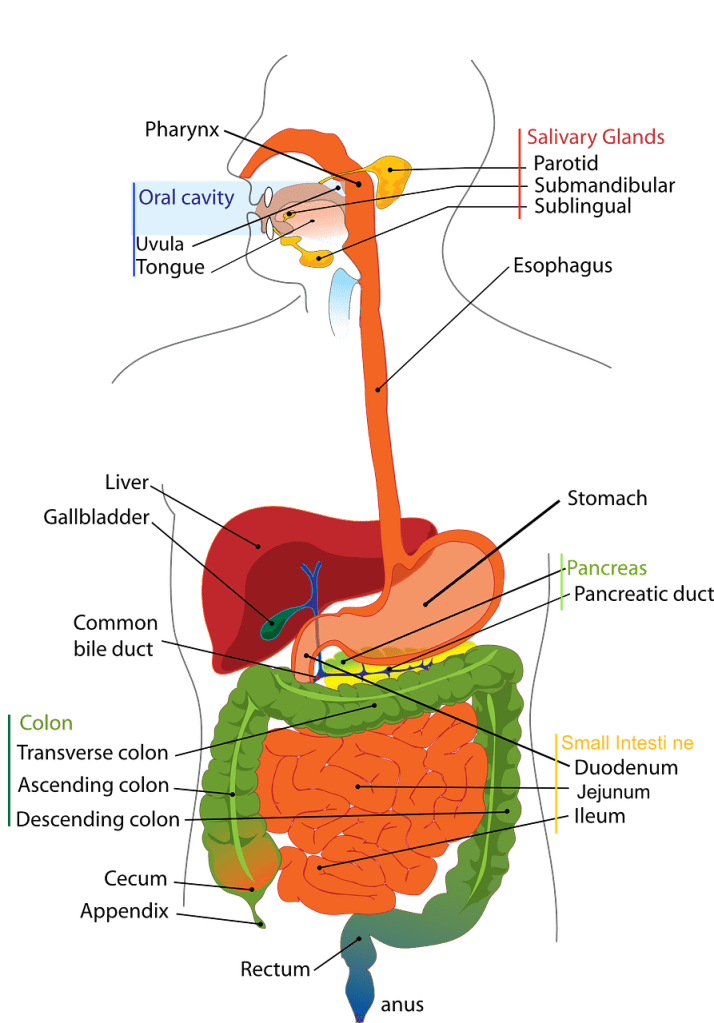
Physicians do not expect IBS to cause bleeding, fever, weight loss, nausea, or vomiting; such symptoms prompt investigation of other conditions, including
- inflammatory bowel diseases-Crohn’s disease and ulcerative colitis
- celiac disease
- gluten sensitivity
- lactose intolerance
- infection
- malabsorption syndromes
The symptoms of IBS are not unique , making diagnosis difficult since it can be confused with other conditions. Women are diagnosed with IBS more often than men, and onset of symptoms after age 50 years is unusual (although it may have been present and unrecognized. ) Children and adolescents can have IBS.
Currently there is no one generally recognized blood test, scan, image, or other diagnostic test that confirms IBS.
Why does IBS happen?
The cause of IBS is still uncertain but gastrointestinal specialists cite several issues that likely contribute.
At one time doctors believed it was due to overactive muscles in the bowel wall, altered motility, leading to the once used name “spastic colon.” Now there are several additional factors that seem to contribute.
One pathway involves the neurotransmitters in the nerves of the bowel that transmit signals from there to the brain and back. A deficiency of these neurotransmitters may be interpreted as pain or may alter gut motility causing diarrhea or constipation.
Changes in the number and type of “gut microflora”, the bacteria that live in the bowel ,has been identified as a possible cause.
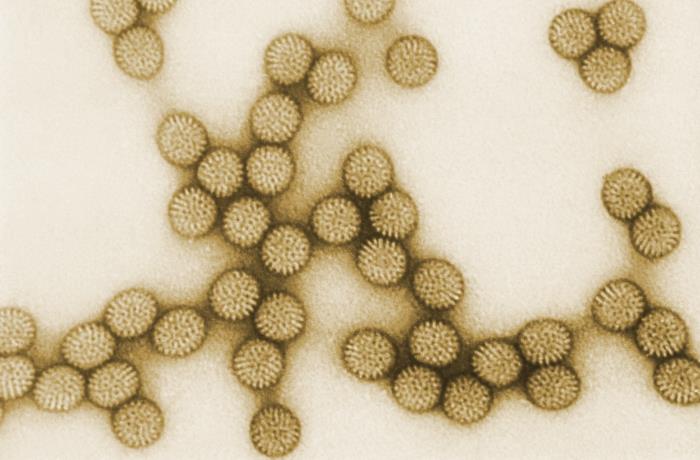
Some people develop IBS after having viral gastroenteritis (infection). The infection may trigger an intense immune response leading to chronic inflammation as the cause of the persistent symptoms.
The stress connection
Beverly Greenwood-Van Meerveld, Ph.D, has devoted much of her career to studying IBS and its relationship to stress. As a profession of physiology at the University of Oklahoma College of Medicine, she has received a grant from the National Institutes of Health to explore how and why stress induces the pain of IBS, and why it seems to differ in women compared to men.
“We know that early-life stress is a risk factor for the development of irritable bowel syndrome later in life. Research has traditionally used males…we need a better understanding of the connection between the brain and the gastrointestinal tract in women.”
Dr. Greenwood-Van Meerveld, OU Medicine magazine, Fall/Winter 2020
Managing IBS
The symptoms of IBS may fluctuate and even go into remission spontaneously, so it can be difficult to definitely know what works and what doesn’t.



Regular exercise, such as a daily walk, and conditioning with moderate to vigorous exercise 3-5 times a week improves digestion and encourages the bowel to move more efficiently.
Adequate and restful sleep helps manage stress that frequently precipitates symptoms.
Mind based therapies
Because of the nervous system involvement, inadequate and unproductive response to life’s stressors will exacerbate symptoms of IBS. Adequately addressing stress plays a key role in managing IBS symptoms. Psychological therapies may be needed- CBT (cognitive behavioral therapy), hypnotherapy, and psychotherapy.
Eating to manage IBS
Experts recommend appropriate food choices and eating habits as basic steps to symptom control.
They emphasize eating meals at regular intervals, limited snacking, and not overeating at any time.
No one food or food group is universally off limits, but some IBS patients do well by avoiding
- alcohol, caffeinated and/or carbonated beverages, and milk
- spicy and fatty foods
- gas-producing foods
- gluten
- artificial sweeteners
- insoluble fiber
Some studies show a low FODMAP diet is especially helpful for bloating whether diarrhea or constipation is the major problem. FODMAP stands for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols short-chain carbohydrates (sugars) that aren’t absorbed properly in the gut.
The UK National Institute of Clinical Excellence (NICE) recommends the low FODMAP diet, whenever general lifestyle and dietary advice fail to relieve symptoms. The guideline further cautions patients to consult health care professionals with expertise dietary management.
FODMAPs are found in various fruits, vegetables, cereals, breads, dairy, and sweeteners so it can be challenging to know what’s acceptable and what’s not. Using a list such as this one or working with a knowledgeable dietician can make it easier to find what works for you.
The Cleveland Clinic offers this FODMAP guide.
Drug therapy for IBS
Non -prescription drugs used for IBS include
- soluble fiber supplements such as psyllium and laxatives for those with constipation
- anti-diarrhea meds for diarrhea
- peppermint oil
(These are affiliate links used to support this blog at no additional cost to you.)
Prescription meds available in the United States specifically for IBS include linaclotide, lubiprostone, eluxadoline , plenecatide,and tegaserod.
Doctors have found short, 2-week course of an antibiotic, rifaximin, helps some patients with IBS, effects that last a few months.
Manipulating the gut microbes
The health benefits imparted by probiotics and prebiotics as well as synbiotics have been the subject of extensive research in the past few decades. These food supplements termed as functional foods have been demonstrated to alter, modify and reinstate the pre-existing intestinal flora.
Probiotics, prebiotics and synbiotics- a review
Because the gut bacteria, or microflora, may be disrupted, manipulating it with prebiotics, probiotics, synbiotics is being tried. These include
Fecal Microbiota Transplantation
An interesting investigational treatment involves fecal transplantation (or bacteriotherapy) , the transfer of stool from a healthy donor into the gastrointestinal tract . Small studies have shown it effective for IBS but the effect may not be long lasting.
Fecal transplantation is currently not routinely performed for reasons other than recurrent C. difficile colitis. More research studies are still needed to determine if fecal transplantation should be performed for other clinical indications. Fecal transplantation for other clinical indications should be considered experimental, and performed only as part of a research study where your safety is closely monitored.

What to do if you think you may have IBS
Monitor your symptoms carefully, keeping a written record, for 1-2 months. Take this to your doctor for an evaluation. However if you have these symptoms, see your doctor immediately.
- bleeding in bowel movements
- unexpected weight loss
- fever
- profuse diarrhea
- persistent failure to pass stool
- severe, disabling pain
A primary care doctor-a family medicine or internal medicine doctor- can evaluate these symptoms initially, and decide if referral to a GI specialist, a gastroenterologist , is needed for more specialized testing.
The American College of Gastroenterology offers these resources for patients with irritable bowel syndrome.
If you have been diagnosed with IBS
Your doctor likely has already recommended some of the measure I have listed above. If not, and your symptoms are not controlled, then you might want to discuss to see if they are appropriate for you.
Remember, this is provided for your information and is not intended as advice or treatment. I encourage you to seek care from your personal physician.
exploring the HEART of health
I appreciate your sharing this post on your social media pages.
Thank you for viewing the advertisements and using the affiliate links that fund this blog; with your help, we can grow, reach more people, and support worthy causes that bring health and wholeness to people around the world.