update February 11, 2025
The CDC website has moved all articles about COVID-19, SARS-CoV-2, into its archives. This post may have CDC links that are no longer active, or have moved. You may be directed to the new link at the CDC website.
In this post I’m sharing some of what I’ve been reading about the COVID-19 epidemic. These experienced, knowledgeable, compassionate physicians share insights to help colleagues as well as patients. I thank them for taking the time to share in the midst of this crisis.
a perspective from China
Since 2016, Laura Jordhen, M.D. has been practicing in Shanghai’s United Family Xincheng Hospital and was chair of infection control for the hospital before becoming chief of its family medicine department in December. In an interview for the AAFP she said,
“(In China now) Things are slowly getting back to normal. Our ear, nose and throat clinic is reopening. Dental is reopening. The number of new confirmed cases is low.
People in Wuhan are still basically isolated in their homes, but throughout the rest of China schools are starting to open up. With still a few cases reported every several days in Shanghai, schools have still not reopened. It’s still very strict social isolation.
Massage, hair cut — any kind of business that involved physical contact or having people close together — was shut down around Chinese New Year, which started Jan 25.”
Read more of Dr. Jordhen’s insights on China’s handling of COVID-19 at
U.S. FP Shares COVID-19 Insights From Practice in China
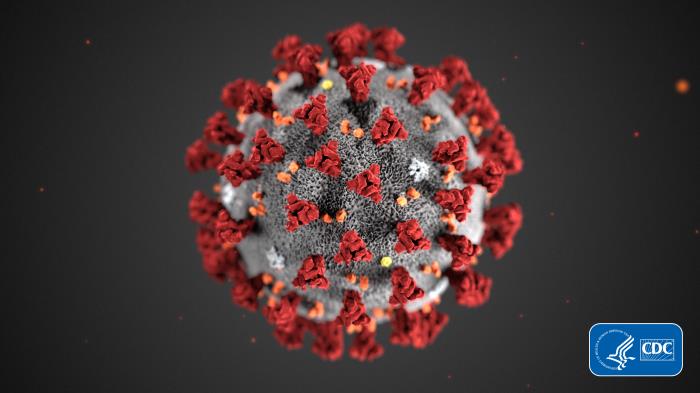
from the National Institutes of Health
On the NIH Director’s blog, Dr. Francis Collins explains social distancing.
“What exactly does social distancing mean?
Well, for starters, it is recommended that people stay at home as much as possible, going out only for critical needs like groceries and medicines, or to exercise and enjoy the outdoors in wide open spaces.
Other recommendations include avoiding gatherings of more than 10 people, no handshakes, regular handwashing, and, when encountering someone outside of your immediate household, trying to remain at least 6 feet apart.
These may sound like extreme measures. But the new study by NIH-funded researchers, published in the journal Science, documents why social distancing may be our best hope to slow the spread of COVID-19. ” Read more at
To Beat COVID-19, Social Distancing is a Must

In A nine-step plan to deal with COVID-19 stress, psychiatrist Dr. Gerard Clancy offers this advice.
“7. Can-do list. Under the current guidelines there are many things we can’t do. With activities out in the community curtailed, this can leave down time. This has allowed us to create a list of what we can do.
This has included reading books, reorganizing the house and watching classic and new movies. It has also included my own version of Master Chef, where I need to cook dinner with what we have left in the pantry. It has been a challenge but also fun.”

Why Doctors and Nurses are Anxious and Angry
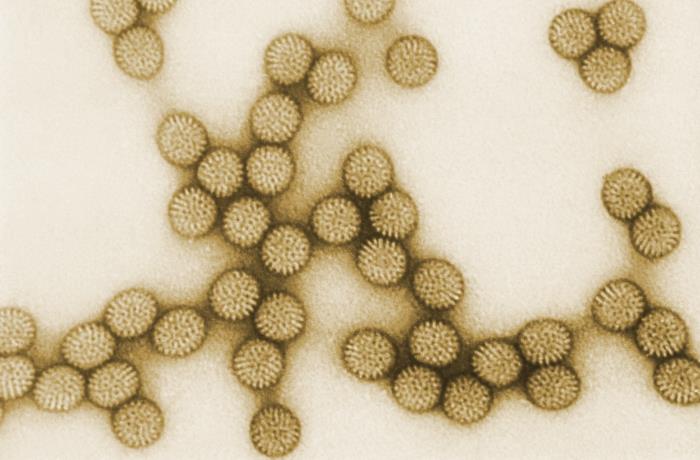
“Every single day for the past six months, I have recommended the flu shot for my patients, and every day a good chunk decline. When I ask why, most can’t articulate an answer. They offer only an inchoate distaste for vaccines, fomented by the oddly contagious anti-vaccine movement.
I remind them that their grandparents would have given their eyeteeth for the vaccines they blithely shrug off. I point out the entirely unnecessary resurgence of measles resulting from a falloff in vaccination rates.”
Dr. Danielle Ofri, a doctor at Bellevue Hospital and a clinical professor of medicine at New York University Grossman School of Medicine, is the author of “What Patients Say, What Doctors Hear” and the forthcoming “When We Do Harm: A Doctor Confronts Medical Error.”
Review your family’s vaccination status at this previous post about vaccine preventable diseases.
exploring the HEART of COVID-19
I’d love for you to follow this blog and follow me on social media.
I share information and inspiration to help you transform challenges into opportunities for learning and growth.
Add your name to the subscribe box to be notified of new posts by email. Click the link to read the post and browse other content. It’s that simple. No spam.
I enjoy seeing who is new to Watercress Words. When you subscribe, I will visit your blog or website. Thanks and see you next time.
Dr. Aletha

My Reader Rewards Club is a great way to earn free books and Bibles for yourself, friends, and family! Your journey to earning free faith-based products starts HERE.
(When you sign up through these links, I can earn free books too.)
As a member, you’ll have access to inspiring literature, Bibles, special promotional offers, and much more. Earning points is easy—you’ll receive 25 points just for signing up!