Your next doctor or one you will see in 10-20 years is likely in medical school or a residency program in a United States medical center right now. Within 1-10 years, they will join the ranks of practicing physicians, as those doctors transition to non-clinical jobs, retire, or die.
These future doctors are training under the most difficult and stressful medical conditions the world has experienced in several generations-a global pandemic of a contagious respiratory pathogen. As such, they will have a unique perspective as they begin and pursue careers as practicing physicians.
More women physicians are training to be doctors.
Medical school enrollment looks more like the general population now.
For 3 years in a row, the number of women entering medical school has steadily increased and exceeded the member of men, while the number of men has decreased.
First year students
- Male students -10, 560
- Female students-11, 612
Total students
- Male students- 42, 735
- Female students- 44, 579
statistics from the Liaison Committee on Medical Education (LCME)

Due to the lag time of the numbers catching up, slightly more men than women graduated in 2020.
- Male graduates- 10,517
- Female graduates-10, 324
Among the 140,000 resident physicians, 64,000 are women.
Large numbers of women medical graduates pursue training in these fields-
- internal medicine
- family medicine
- obstetrics/gynecology
- pediatrics
- dermatology
- geriatrics
- neurology
- ophthalmology
- psychiatry
But ethnic diversity is still low among physicians in training.
The nation’s medical schools need more diversity. The factors that create racial and ethnic inequities in other areas of society impact medical education also.
In 2019-2020, white students made up the majority of medical students although both the number and percentage have decreased, while the number of all other groups has increased.
Based on self identification, the Association of American Medical Colleges reports students are
- White-46,205
- American Indian/Alaska Native -199
- Asian-20, 836
- Black /African American-6,783
- Hispanic, Latino, Spanish Origin-6,063
- Native Hawaiian/Pacific Islander-76
- Other-1,776
- Multiple-8,621
- Unknown-892

After medical school, graduates enter residency training for a specialty. Medical residents, both male and female, are still predominantly white. Based on self-identification, race and ethnic origin of medical residents in 2019 is
- White-76,964
- Black-8009
- Hispanic(any race)- 11,860
- Asian-37,477
- Multiracial- 4740
- Unknown/other-13,135
- Native American/Alaskan-190
- Native Hawaiian/Pacific Islander-101

Citizenship of physicians in training
Through its certification program, the Educational Commission for Foreign Medical Graduates (ECFMG) evaluates students who attend a non U.S. medical school.
After ECFMG certification, physicians who wish to practice medicine in the United States must complete an accredited residency training program in the United States or Canada. This process will take at least 3 years. The physician will have to complete a residency program regardless of the training he or she has received overseas.
In 2019, 71% of 140,000 resident physicians were native born U.S. citizens. The rest were
- Naturalized citizens- 8%
- Permanent residents- 5%
- Various permits-7%
- Refugee/displaced persons-0.1%
- Unknown status -7%
Goals of new physicians
“Most students, including minority, disadvantaged, and marginalized students, enter medical school pursuing a lifelong dream of practicing medicine with little sense of projected incomes or what specialty they would like to pursue.
Most specialty choices are likely based on social, educational, and health care experiences; experiences in medical school; and the prospect of a 30-plus-year career in an area of medicine that provides a level of personal comfort, support, and fulfillment.”
Thomas B. Free Medical School Tuition: Will It Accomplish Its Goals? JAMA. 2019;321(2):143–144. doi:10.1001/jama.2018.19457
The specialization of medical care- the good and the bad
On Match Day, occurring mid March every year, graduating medical students learn which residency program they will enter through the National Resident Matching Program , which “matches” them with available positions in residencies at medical centers all over the United States. A kind of medical “matchmaking” you could call it.
For many students, Match Day has become a quasi graduation celebration, with friends and family in attendance to share the “reveal”. In 2020 due to the viral pandemic, they had to settle for celebrating virtually.
This matching process determines who will care for our medical needs in the next 30-40 years; our family physicians, internists, pediatricians, general surgeons, obstetricians, and the multitude of other medical specialties. Most doctors will continue in the same specialty their entire career, although some switch after a few or many years.

Some medical students know what speciality they want to pursue before they enter medical school, while others decide after trying the different types of medicine while students. We still have the traditional specialities that most students enter- (there are also many subspecialities under each of these categories.)
Primary care
- Family medicine
- Internal medicine -(adult medicine)
- Pediatrics-children and adolescents
- Obstetrics/Gynecology- care of women’s health and pregnancy
Surgical specialities
- General Surgery- surgery on skin and internal organs
- Orthopedics-bones and joints
- Otorhinolaryngology- ear, nose, throat
- Ophthalmology-eyes
- Neurosurgery-the brain, spine, nerves
- Plastic and Reconstructive surgery
- Cardiac and vascular surgery
Others
- Dermatology-skin
- Psychiatry-mental health
- Anesthesiology-surgical sedation and pain relief
- Emergency medicine- emergencies and trauma
- Radiology- xrays and other imaging-CT, MRI, US
- Pathology-laboratory medicine
- Allergy
- Physical medicine and rehabilitation
- Oncology-treatment of cancer
- Integrative and complementary medicine
As medical care has become more complex and technological, so have the specialties of physicians. This has produced a plethora of new highly specialized fields of practice.
- Sleep medicine
- Medical genetics and genomics
- Pain management
- Geriatrics- care of the elderly
- Palliative care-managing diseases that cannot be cured and are likely terminal
- Hospital medicine-care of patients admitted to a hospital
- Critical care medicine-care of patients in an ICU (intensive care unit)
- Aerospace medicine
- Wound management
- Medical informatics – use of computers and medical software in medicine
- Bariatrics- treatment of obesity with or without surgery
- Sports medicine-treatment of athletic injuries and fitness training
- Transplant medicine- surgery to transplant organs and after care
- Addiction medicine
A 2018 viewpoint in JAMA suggested that we need a new specialty, virtual medicine, to describe physicians who treat patients through a virtual medium, telemedicine or web based, on a computer or a mobile app.
The onset of the SARS-CoV-2 pandemic forced physicians to find alternate ways of delivering care. Even emergency rooms and urgent care clinics were forced to redesign their work flow to care for ill and injured patients while not enabling spread of the virus to staff and other patients.
The risk of contagion halted most non-emergent in person care but physicians’ offices soon implemented alternate means of reaching out to patients-curb side consults, telephone, and virtual visits using smart phones and computers.
Health plans, including Medicare, supported these alternate delivery services with loosened restrictions on paying for virtual care.
Both patients and doctors benefited by this new model which seems destined to persist past the pandemic.

The problem-overspecialization in medical care
According to the New England Journal of Medicine,
“the progress of biomedical science is a major factor in the emergence of new subspecialities. There are some patients who benefit from highly focused knowledge and skills.”
All of these specialities mean more medical knowledge and experience will be available to both treat and prevent a diverse and growing variety of disorders.
Today’s new specialist has high degree of expertise in their field, making them better able to treat your problem in the most efficient, effective, safest way.
But with a more narrow focus of experience, that doctor may be less familiar with other aspects of your medical status.
You may find your specialist recommends more testing, which may lead to more treatment some of which may not necessarily improve outcomes.
More specialized testing and treatments may increase the cost of medical care.
Dr. Sandeep Jauhar addresses this issue in this article from Time.
One Patient, Too Many Doctors: The Terrible Expense of Overspecialization
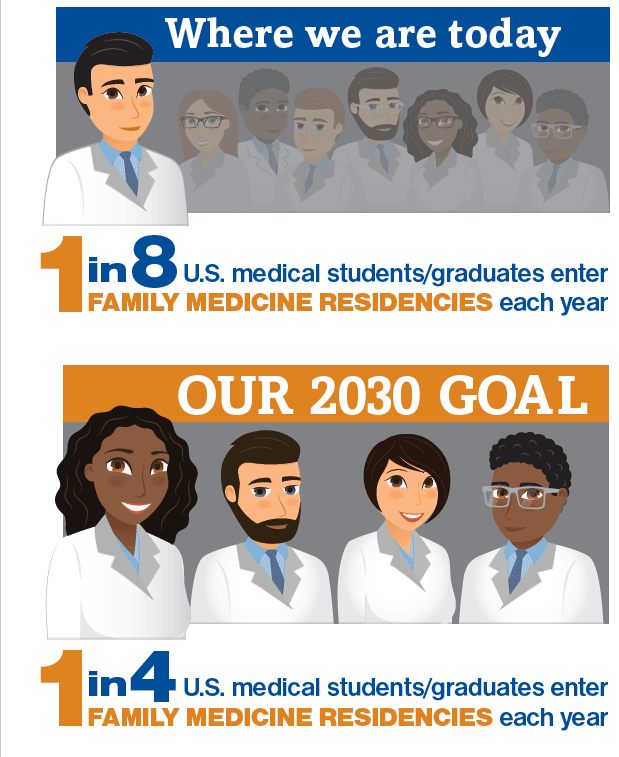
The challenge-increasing the primary care workforce
Primary care physicians can close this gap by coordinating care, especially for complex patients.
4,335 medical students and graduates matched to family medicine residency programs in 2020, the most in family medicine’s history as a specialty, and 487 more than 2019.
Family physicians make up the majority of the primary care physician workforce and mirror the geographic distribution of the U.S. population—practicing in rural and urban underserved communities
“Public health issues like the pandemic the world is experiencing now underscore the importance of a strong foundation in primary care at the front lines surveilling and treating the community.”
Gary LeRoy, MD, president of the American Academy of Family Physicians.
I specialize in Family Medicine
I’ve often been asked ,”Why didn’t you specialize?” My answer, “I did. I specialize in Family Medicine.”
Once called “general practice”, Family Medicine is now a recognized specialty, requiring a residency and certification by the American Board of Family Medicine.

Lightstock photos
Unless otherwise stated, the doctor photos in the post are from the Lightstock.com collection . Get a free 30 day trial at this affiliate link. (This blog can earn a commission if you buy photos which helps support the mission of Watercress Words.)
exploring the HEART of health care education
my regards, Dr. Aletha