Parents and educators in my state have been debating the merits of standardized testing for school children and maybe where you live also. And it’s not just a question for children, adults can be subjected to professional testing also.
After I finished my family medicine residency, I took an 8 hour paper multiple choice written exam to become certified by the American Board of Family Medicine (ABFM). The tests were held at several large cities across the United States.
Every 10 years I tested to re-certify. (Originally it was every 7 years) and I always had to travel at least 500 miles to one nearest my home. Eventually the Board transitioned to a computer based exam taken at a local testing center, still 8 hours long.
The purpose of board certification is to make sure you, the patient, are getting the best care possible from a physician. According to the ABFM,
We promise that board certification means that the family physician you choose for your care meets high standards.
American Board of Family Medicine, ABFM

In 2018 they offered something new- doctors could take the test on their own computer or tablet whenever and wherever they chose, called The Family Medicine Certification Longitudinal Assessment (FMCLA)
Launched in December 2018 as a pilot program, FMCLA quickly earned an overwhelmingly positive reputation as the preferred option for most physicians and was approved for permanent use in April of 2021.

This exam consists of 25 questions posted quarterly over 3 years, with a 5 minute time limit for each question . Besides being able to take the exam in my pajamas, I can research the answers online if I need to-as long as I can do it in 5 minutes. The rules prohibit me from discussing the questions with another person, based on an honor system that I attest to before beginning each session. Being able to look up information is more like actual medical practice.
More aligned with adult learning principles, this approach allows for use of references and promotes greater retention of new knowledge to be applied in daily practice.
ABFM web site
You can learn more about the value of board certification at this link
American Board of Family Medicine Patient Page
While board certification is a voluntary process, many organizations prefer or require the physicians they hire or work with to be board certified.
Take an “exam” designed for patients
I thought I would give you a taste of what I am doing by creating a patient certification exam for you. The rules prohibit me from sharing actual test questions so I have written my own, in simple medical terms, but using a format similar to the questions I answer.
When I answer questions, I get immediate feedback if my answer was right or wrong, with an explanation and a reference. So I have done the same for you. In this case, the reference is from a blog post I have written.
There’s no time limit for each question and for this exam, feel free to discuss your answers with someone else, I encourage you to. Choose the single best answer. Check at the end for the correct answers.
I had fun writing these questions so I hope you have fun answering them. Good luck! I hope you pass.
Question 1
A woman came to her doctor with a skin rash soon after starting to take a new medication. The medication is most likely
- An Antidepressant
- A blood pressure lowering drug
- An anti-inflammatory drug
- An antibiotic
Question 2
A 25 year old woman notices that the skin on her face has darkened over the past several months. This condition is called
- Melasma
- Eczema
- Psoriasis
- Tinea
How common meds hurt skin
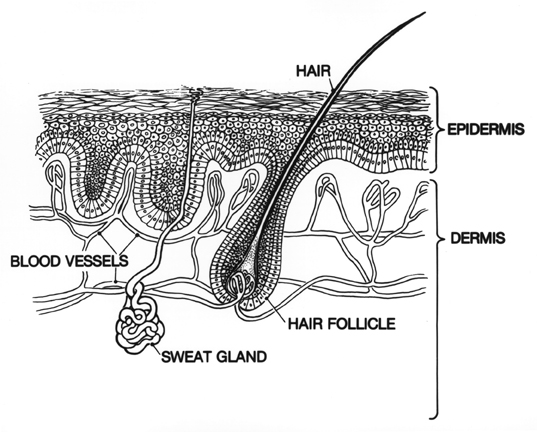
Question 3
A mother brings her 8 year old daughter to her family doctor. The child has a cough, runny nose, and mild sore throat. Her temperature is 100.2 degrees. The doctor diagnosed the illness as a cold, or upper respiratory infection and explains this is caused by a virus. She does not prescribe an antibiotic because
- The child is allergic to penicillin
- The family does not have health insurance
- The mother has left over antibiotic from another child at home.
- An antibiotic will not help an infection caused by a virus.
How to cope with winter illness
Question 4
A 30 year old woman comes to her doctor because she is losing an excessive amount of hair. She is afraid she will become bald. Most likely she
- Started using a cheap shampoo
- Delivered a baby
- Needs vitamins
- Should investigate hair implants
Effective solutions if you experience hair loss
Question 5
Dr. Oglesby believes that certain medications should be used more often because of their benefit to patients. These drugs include all except
- Antibiotics
- Vitamins
- Sleeping pills
- Stop smoking drugs
7 underused drugs
Question 6
A young man who is a computer programmer has difficulty falling asleep. His doctor may recommend
- Buy a new mattress
- Taking a sleeping pill an hour before bedtime
- Regular exercise and relaxation techniques
- Watching television until he falls asleep
Expert advice to sleep

Question 7
Author and motivational speaker Nick Vijucic was born with amelia. This term means he lacks certain parts of his body which are his
- Limbs
- Eyes
- Ears
- Teeth
Light and life without limbs
Question 8
A woman sees her doctor because she researched her symptoms online and believes she has endometriosis. She thinks this because
- She does not have regular periods.
- She had a miscarriage.
- She has not been able to get pregnant.
- Her sister has it.
Question 9
The HPV (human papilloma virus) causes cancer. Vaccination against this virus decreases the risk of cancer of the
- Cervix
- Uterus
- Breast
- Ovary
Women’s health update
Question 10
Kristin Chenoweth, Tony Award winning actress and singer, suffers from Meniere’s syndrome. She was born in a small town in Oklahoma named
- Muskogee
- Broken Arrow
- Ada
- McAlester
Kristin Chenoweth– a review of her memoir

ANSWERS TO QUESTIONS
- The most common drug that causes a skin rash is an antibiotic.
- Melasma
- Antibiotics do not help a cold or any other viral infection
- delivered a baby; hair loss is common after pregnancy
- Stop smoking drugs can be useful to help smokers quit. The other drugs listed are often overused.
- Exercise and relaxation can improve one’s sleep.
- Nick was born without limbs.
- Infertility is a common symptom of endometriosis.
- Cancer of the cervix is caused by the HPV virus.
- Broken Arrow. The other Oklahoma towns produced Carrie Underwood, Blake Shelton, and Reba McIntyre.
testing the HEART of health
Thanks for testing your knowledge with this first ever Watercress Words Certification Exam. If you liked it, let me know, maybe we’ll do it again.
Dr. Aletha
RoboForm Password Manager. What I use to manage passwords.
Go to this link to try RoboForm Free;
if you like it you can upgrade to RoboForm Everywhere version with all the features
With Roboform, you will have one less thing to feel stressed about. (affiliate link)



